Open Enrollment Digital Listening Bulletin #2
Cost-Shifting Fatigue Sets In As Higher Healthcare Costs Persist During Open Enrollment
Welcome to week two of our Fall 2019 Group Benefits Open Enrollment Digital Listening Bulletin. In this bi-weekly e-mail, we take a look at the trends, conversations, and themes that we are seeing dominate the group benefits discussion over the last two weeks as many carriers, brokers, heads of HR, and employees go through open enrollment season.
Even more of the benefits conversation turned to the rising costs of the healthcare portion of group benefits over the last two weeks as the reality of 2020 plan options settles in and employers and employees are both faced with rising plan costs, decreased benefits-or both.
Reality Settles In
According to the KFF 2019 Benchmark Employer Health Benefits Survey released in late September, annual family premiums rose 5% in 2019, while worker’s wages rose 3.4% and inflation rose 2% over the same period. We appear to be on track for another 5%-10% increase for 2020.
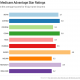
Employers large and small are actively seeking new ways to reduce benefit costs. FedEx just announced significant changes to its benefits program for 2020, including a surcharge for working spouses of employees, end out-of-network coverage and phase out domestic and civil union partner benefits as it struggles to maintain a strategy of keeping cost increases below the national average.
Others seem resigned to the current situation: “Just went through our company health insurance renewal. As a CFO, you know when you’ve been beat into submission when the health insurance companies raise your premiums ONLY 10% and you’re happy about it.”@MonetaryWonk
Some surveys are now beginning to actively track “Cost-Shifting Fatigue”—the perceived ability of employers to continue to ratchet up employee cost-sharing arrangements by increasing employee premium contributions and plan-sharing responsibilities, resulting in higher deductibles and out-of-pocket maximums. Using a 10-point scale, where 1 means the employer has a minimum cost-shifting fatigue and 10 means the employer has reached its limit of shifting costs to employees and is now considering to no longer offer health coverage, a recent Iowa Benefits Study found that Iowa employers were at a weighted average of 3.5. Iowa employees can expect to see increased cost shifting for a while!
They should run an employee-based “Cost-Shifting Fatigue” survey. I think likely it would be much closer to 10!
- “Currently I pay $87.60 a month for amazing health insurance through my employer. They are getting rid of the health plan I have had since I started here and going with a new plan. “Most employees will see minimal premium increases…” I guess I’m not most. $186.45 1/1/20.” @norcalcop
- “On top of this it’s the employee, not the employer who pays the monthly premiums in most cases, which means a pay cut from your paycheck to fund medical insurance which is really a complete ripoff with high premiums and co-pays and extremely poor coverage that might be denied for the most specious of reasons. Health insurance my ass, it’s a grifting con.”
The June HRA rule has provided an “out” for smaller employers and new options for employees in the individual market. Some are predicting this is the beginning of the end of employer-based health coverage and that carriers and brokers should be thinking about a new model in order to survive the “coming tsunami”.
The Platform-as-a-Channel Wars
A quick search on G2 this morning for “Benefits Administration Software” brought up 180 listings—180! Software Advice lists 210 providers.
Carriers and brokers are continuing to try and effectively navigate a complex and rapidly changing technology landscape this openenrollment season as new competitors emerge, new partnerships announce, private exchanges proliferate, compliance requirements evolve and data standards emerge.
The significance of the BenAdmin “Platform-as-a-Channel” as a key component of the Group Benefits go-to-market model is increasing as carriers, brokers and employers try to take friction out of the group benefits process through technology and expand their coverage and choices through platforms.
With a limited set of technology and partnership bets that can be placed and effectively managed, carriers and brokers must be focused in their strategy, hedging those bets across multiple models and constantly evaluating their performance as winners (and losers) emerge in the technology consolidation that is coming as platforms compete for the requisite scale that will enable long-term sustainability.
Aflac announced earlier this month that it will make its voluntary benefits available through PrismHR’s platform and Insurance Alliance to their HRO Partner network. “The PrismHR and Aflac partnership, managed by Alterity, will not only offer employees best in class benefits, it will also provide for a more streamlined administrative experience.” Less friction, more coverage in the small business market.
SunLife is hedging its bet on Maxwell Health last year by expanding its relationship with other BenAdmin tech platforms as well. On October 23rd, they announced their partnership with Employee Navigator. “Sun Life is committed to simplifying the benefit administration experience for our brokers, employers and members,” said Joi Tillman, vice president of Voluntary Benefits at Sun Life Financial U.S. “By partnering with technology platforms like Employee Navigator, we can make sure the experience fits with the needs of different employers.” Again, less friction, more coverage.
Ultimately carrier and brokers will need to work across most—if not all—remaining platforms in tomorrow’s API world. Managing a data-driven customer experience in this model will be critical to future-proof success. The PaaC wars will continue!
Help! I Need Somebody, Not Just Anybody
In a recent survey, MetLife found that employees dread open enrollment nearly as much as renewing their license. Our research has shown that employees want the ability to interact with a well-prepared, well-versed and accessible individual when it comes to their benefits administration. Tools help, but at the end of the day, most employees still prefer the human touch.
Many employers are taking a more personalized approach to benefits communication—throughout the year, not just during openenrollment. Nebraska Medicine has had great success using trained benefit communication specialists to meet with each of their 9,000 employees to make sure they are selecting the right plans.
As competition for the Benefits wallet share heats up, forward-thinking brokers and carriers will be leveraging data and customer insight to help employers personalize and tailor the benefits conversation, and to help employees optimize their benefits across categories.